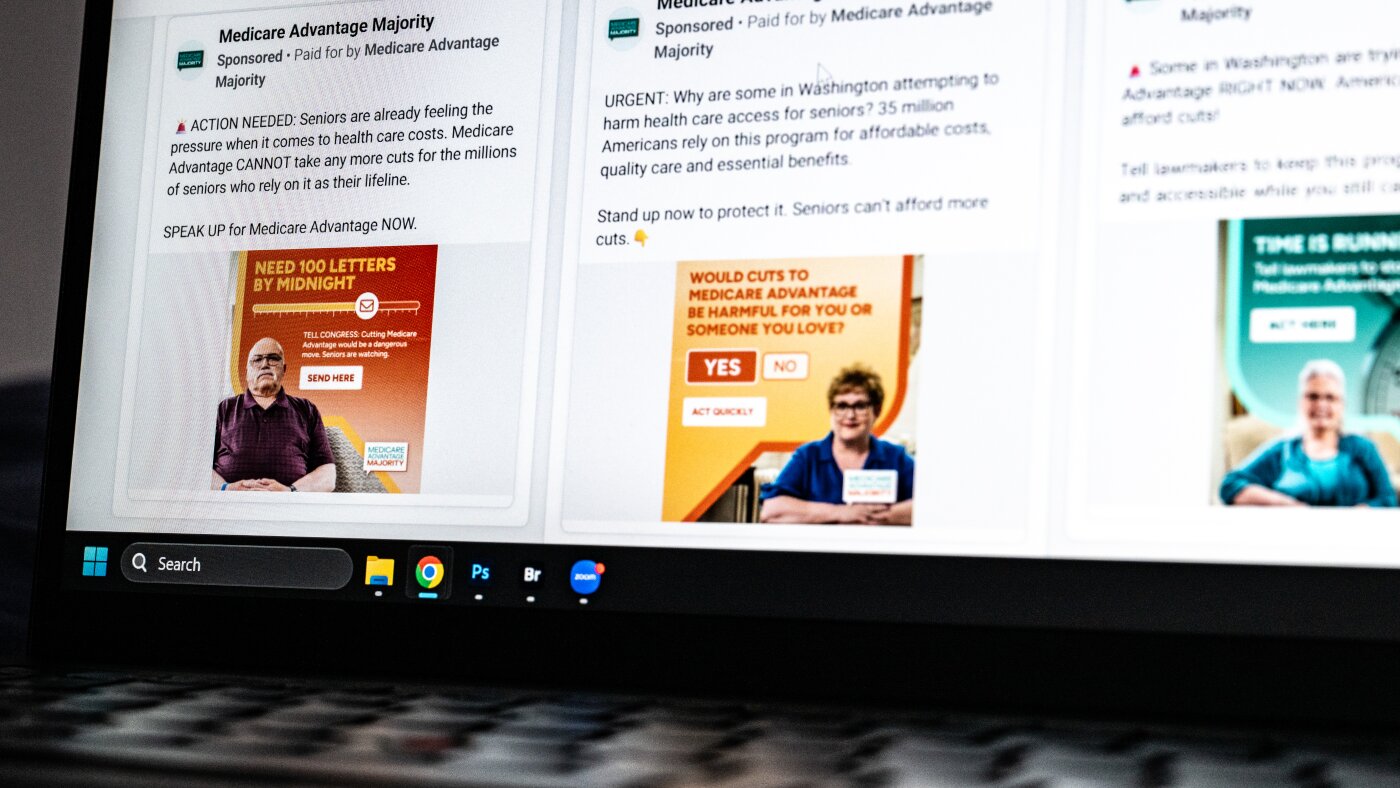
"About 83% of the comments are identical to a letter that appeared on the website of a secretive advocacy group called Medicare Advantage Majority, a data analysis by KFF Health News has found. The 'dark money' group does not reveal its funders or much else other than to say it is 'dedicated to protecting and strengthening Medicare Advantage' and is 'powered by hundreds of thousands of local advocates nationwide.'"
"The group has spent more than $3.1 million on hundreds of Facebook ads since September 2024, according to Facebook's Ad Library, a database of the social media company's online ads. There's no doubt health insurers are unhappy with a January proposal from the Centers for Medicare & Medicaid Services, or CMS to keep Medicare Advantage reimbursement rates essentially flat in 2027—far less than they expected from the Trump administration."
"Medicare Advantage plans differ from traditional Medicare because private insurance companies administer them. The insurance plans enroll about 35 million members, more than half the people eligible for Medicare. The plans offer things like vision and drug coverage, but Medicare Advantage insurers restrict the hospitals and doctors that patients can use and require prior approval for various procedures."
Medicare Advantage Majority, a secretive advocacy group with undisclosed funders, coordinated a campaign resulting in over 16,300 nearly identical comments on a federal government website opposing CMS's proposal to keep Medicare Advantage reimbursement rates flat in 2027. Analysis by KFF Health News found 83% of comments matched a letter from the group's website. The organization spent over $3.1 million on Facebook ads since September 2024 while claiming to represent grassroots advocates. Medicare Advantage plans, administered by private insurers, cover 35 million members—over half of Medicare-eligible Americans. The plans offer supplemental benefits but restrict provider networks and require prior authorization. CMS is expected to announce its final reimbursement decision by early next month following the public comment period.
#dark-money-advocacy #medicare-advantage #astroturf-campaigns #healthcare-policy #cms-reimbursement-rates
Read at www.npr.org
Unable to calculate read time
Collection
[
|
...
]